OPIATE ADDICTION

22-year-old Keith Richards in 1965, when he sort
of looked and dressed like Liam Gallagher of Oasis Opium, heroin, morphine and codeine and other opiates are all addictive — a psychological and sometimes physical attachment to a substance that drives someone to take it even when using it can be very destructive. Some doctors view addiction as manipulation of the brain to make it feel that the drug a person is addicted to is necessary for survival. There are an estimated 40 to 50 million heroin and opium addicts worldwide. In the United States, there are about 600,000 heroin addicts, about half of them in New York City — or at least that was so at one time.
Addiction is caused when drug users no longer take the drug to feel good but take it to avoid feeling bad. Long-term opiate use causes users to build up a tolerance to a drug as endorphin receptors respond less and less to it. At this stage users get little pleasure from other things in their life. The drug becomes the only source of anything resembling pleasure. Without it they feel anxiety, irritability and depression.
Heroin, cocaine, amphetamines, alcohol and nicotine are regarded as the five drugs hardest to give up. As of the late 2000s, 22 million Americans were hooked on at least one of these substances. Researchers are studying the long-term effects of opioid addiction on the brain. Studies have shown some loss of the brain’s white matter associated with heroin use, which may affect decision-making, behavior control, and responses to stressful situations.
See Separate Article OPIODS: TYPES, EFFECTS AND DANGERS factsanddetails.com HISTORY AND USE OF OPIUM factsanddetails.com ; HISTORY OF HEROIN factsanddetails.com ; HEROIN USE factsanddetails.com ; FENTANYL AND PRESCRIPTION OPIOIDSfactsanddetails.com
Websites and Resources: U.S. Drug Enforcement Administration (DEA) justice.gov/dea/concern ; Vaults of Erowid erowid.org ; United Nations Office of Drugs and Crime (UNODC) unodc.org ; Wikipedia article on illegal drug trade Wikipedia ; Frank’s A-to-Z on Drugs talktofrank.com ; Streetdrugs.org streetdrugs.org ; Illegal Drugs, country by country listing, CIA cia.gov/library/publications/the-world-factbook
Books: “Buzzed” by Cynthia Kuhn Ph.D. Scott Swartzwelder, Ph.D., Wilkie Wilson Ph.D. of the Duke University Medical Center (Norton, 2003); “Consuming Habits: Drugs in Anthropology and History” by Goodman, Sharratt and Lovejoy; “Drug War Heresies: Learning from Other Vices, Times and Places” by Robert MacCoun and Peter Reuter (Cambridge University Press). Books on Opium: “Opium, a History” by Martin Booth (1998, St. Martin's Press); “Opium: A Portrait of the Heavenly Demon” by Barbara Hodgson (Chronicle)
Description of an Opium Addict

Rolling Stones in 1971 Describing her opium addict grandfather, a gainfully-employed mason in Singapore, Lavinia Chang told Time, "Nearly everything he earned was spent on feeding his habit. When he had money, he would smoke better-garde opium; when funds were low, he would buy the buy the poor-grade pellets that he swallowed several times a day. With no savings, there were times in between jobs when he could not even afford the pellets. That is when withdrawal symptoms kicked in."
"It would start off like a cold, with teary eyes and a runny nose, followed by involuntary twitches in the face. His hands would start to shake, so he could not even have a drink without spilling it. At the full-blown 'cold turkey' stage, he would lock himself in his room and push the key out from under the door. We could hear his desperate groaning from within but knew there was nothing we could do to help. I don't know how long he stayed locked up; it seemed like a very long time."
There were bad memories of "him shivering under a blanket at midday, with mucous dripping from his nose and saliva drooling from his opened mouth into a perspiration-soaked pillow...When he became quiet again, my mother or one of my aunties would go in and help him out of bed...Though he seemed barely conscious, I knew he was fully aware of his suffering. Watching we suffered too. That's one of the most cruel side effects of substance abuse. It produces a host of silence victims: parents, siblings, partners, children, grandchildren and friends."
When she was 12 her grandfather told her, "I was foolish and I thought I was buying a happier life. It was an escape. twenty cents a day helped me get through the horrible working conditions. I thought if I worked harder and longer, I would earn more for my family. But the price shot up once I became dependent. It has cost me my life. I never thought I would become addicted."
Heroin Addiction

Keith in 1988
Heroin is one of the most addictive substances known to man. It is both physically and psychologically addictive. Users have an intense craving for the drug and seem willing to do almost anything to get it. The writer William Burroughs described heroin as the ultimate product because "the client will crawl through a sewer and beg to buy."
People who regularly use heroin often develop a tolerance, which means that they need higher and/or more frequent doses of the drug to get the desired effects. A substance use disorder (SUD) is when continued use of the drug causes issues, such as health problems and failure to meet responsibilities at work, school, or home. An SUD can range from mild to severe, the most severe form being addiction.[Source: National Institute on Drug Abuse, National Institutes of Health, U.S. Department of Health and Human Services, June 2021]
Heroin addicts are known as junkies. They often need to get heroin every few hours to avoid the onset of withdrawal. Their life often revolves around doing heroin and getting the money to purchase it. Many turn to crime or prostitution. Theft committed to raise money to buy heroin is the major cause of crime in cities the United States. In the Netherlands, about 5,000 of the country's 25,000 hard drug addicts are responsible for about half of all petty crimes.
Truly becoming an addict requires the use of large does over a long period of time. Percent of users who are dependent: 34 percent (compared to more than 80 percent for nicotine). The recovery rate is 40 to 50 percent, compared to 90 percent for cocaine.
Heroin Withdrawal

heroin
A long period without the drugs leads to withdrawal. Withdrawal is an intensely unpleasant and potentially life-threatening experience. Addicts suffer from diarrhea, vomiting, painful stomach cramps, and headaches and, sometimes, convulsions. They often are chronically nauseous, are hypersensitive to pain, ache all over, hallucinate and get the shakes and sweats. One heroin addict told Newsweek, “It was like there were ants crawling up my bones; my nose and eyes were running; my whole body hurt.”
Withdrawal may occur within a few hours after the last time the drug is taken. Major withdrawal symptoms peak between 24–48 hours after the last dose of heroin and subside after about a week. However, some people have shown persistent withdrawal signs for many months. .Those who are addicted to heroin and stop using the drug abruptly may have severe withdrawal. Withdrawal symptoms — which can begin as early as a few hours after the drug was last taken — include: 1) restlessness; 2) severe muscle and bone pain; 3) sleep problems; 4) diarrhea and vomiting; 5) cold flashes with goose bumps ("cold turkey"); 6) uncontrollable leg movements ("kicking the habit"); 7) severe heroin cravings. [Source: National Institute on Drug Abuse, National Institutes of Health, U.S. Department of Health and Human Services, June 2021]
PBS on the classic set of opiate withdrawal symptoms: About eight to twelve hours after the last heroin use, an addict's eyes begin to tear and he/she starts to experience flu-like symptoms: sneezing, weakness, depression, muscle cramps, nausea, vomiting, diarrhea. The symptoms increase in severity over two to three days. Within a week to 10 days the illness is over. The phrase 'cold turkey' probably comes from the appearance of goose bumps all over the body, which resembles a plucked turkey. Muscle spasms in the legs produce kicking movements, and this may be the derivation of the expression 'kick the habit.' In contrast to opiates, cocaine withdrawal is much less dramatic, characterized by sleep disturbances and depression. Some researchers believe that no real withdrawal syndrome exists for cocaine, marijuana, amphetamines, and hallucinogens, since withdrawal symptoms appeared to be psychological rather than physical. At the opposite end of the spectrum are alcohol and barbiturates (downers). For reasons not fully understood by scientists, withdrawal from alcohol and barbiturates, both central nervous system depressants, can be fatal. [Source: PBS, WGBH, Frontline 1998]

brown sugar heroin
Describing withdrawal in his book “Junkie” , William Burroughs wrote: “The last of the codeine was running out. My nose and eyes began to run, sweat soaked through my clothes. Hot and cold flashes hit me as though a furnace door was swinging open and shut. I lay down on the bunk, too weak to move. My legs ached and twitched so that any position was intolerable, and I moved from one side to another... Almost worse than the sickness was the depression that goes with it. One afternoon I closed my eyes and saw New York in ruins. Huge centipedes and scorpions crawled in and out of empty bars and cafeterias and drug stores...Weeds were growing through cracks and holes in the pavement. There was no one in sight. After five days I began to feel a little better.”
Heroin Disorder
Repeated heroin use often results in heroin use disorder — a chronic relapsing disease that goes beyond physical dependence and is characterized by uncontrollable drug-seeking, no matter the consequences. Heroin is extremely addictive no matter how it is administered, although routes of administration that allow it to reach the brain the fastest (i.e., injection and smoking) increase the risk of developing heroin use disorder. Once a person has heroin use disorder, seeking and using the drug becomes their primary purpose in life. [Source: National Institute on Drug Abuse, National Institutes of Health, U.S. Department of Health and Human Services, June 2018]
In the U.S., Among people aged 12 or older in 2020, an estimated 0.2 percent (or about 691,000 people) had a heroin use disorder in the past 12 months. [Source: 2020 National Survey on Drug Use and Health]
Heroin Addiction Treatments
methadone Physical addiction to the drug takes about a week to get over. Withdrawal can be minimized by slowly tapering the dose over days or weeks. Symptoms of withdrawal can be treated with medications such as clonidine for hyperactivity and beznodiazepoen for anxiety. Psychological addiction can last a lifetime. Abstinence allows dopamine receptors to eventually recover to normal. One of the biggest problems with treating addictions is preventing relapses. Recent studies show that the drugs like heroin can have long-lasting effects on brain activity that can remain for months or even years after an individual has stopped doing drugs and these changing can trigger cravings that cause an addict to relapse.
A variety of effective treatments are available for heroin use disorder, including both behavioral and pharmacological (medications). Both approaches help to restore a degree of normalcy to brain function and behavior, resulting in increased employment rates and lower risk of HIV and other diseases and criminal behavior. Although behavioral and pharmacologic treatments can be extremely useful when utilized alone, research shows that for many people, integrating both types of treatments is the most effective approach. [Source: National Institute on Drug Abuse, National Institutes of Health, U.S. Department of Health and Human Services]
The many effective behavioral treatments available for opioid use disorder can be delivered in outpatient and residential settings. Approaches such as contingency management and cognitive-behavioral therapy have been shown to effectively treat heroin use disorder, especially when applied in concert with medications. Contingency management uses a voucher-based system in which patients earn "points" based on negative drug tests, which they can exchange for items that encourage healthy living. Cognitive-behavioral therapy is designed to help modify the patient’s expectations and behaviors related to drug use and to increase skills in coping with various life stressors.
It is important to match the best treatment approach to meet the particular needs of each individual patient. There are medicines being developed to help with the withdrawal process. The FDA approved lofexidine, a non-opioid medicine designed to reduce opioid withdrawal symptoms.
Tough Love Buddhist Treatment for Addicts in Thailand

Buddhist monks The monastery at Wat Tham Krabok runs a treatment center for heroin and opium addicts that combines counseling, herbal therapy and job training. Tham Krabol Monastery north of Bangkok gives heroin and opium addicts a free 10-day treatment that begins with a vow to Buddha to stop using drugs and the downing of a herbal concoction that causes them to vomit immediately and "clear poisonous drug residue from the body and helps eliminate the physical desire for drugs." The monks have treated more than 100,000 addicts with a variety of concoctions and herbal pills and steam baths and claim a 70 percent success rate.
For the most part, treatment and counseling service for addicts is minimal. Government money goes primarily into enforcement and education not treatment. Addicts are generally looked upon with disgust rather than sympathy and people don’t want to see tax-payer money wasted on them. Overcoming drug addiction is viewed as matter of will and discipline and something an addict has to deal with himself. Treatment centers are generally like boot camps or prisons, and even these places can’t keep up with the demand.
Alcoholics Anonymous-type programs are available in Asia but not widely used. The prisons are filled with addicts and small time dealers. About 70 percent of the 200,000 inmates in Thai prisons are there on drug-related offenses. One in five are women. Many of them have small children that are in prison with them.
The few drug rehab centers in Myanmar have waiting lists and treat addicts as young as 13. At one prison in Muse addict in leg irons and wooden cages are forced to sit in the lotus position for excruciatingly long periods of time.
Drug Treatment, Chinese Style
Drug treatment under the Communist has traditionally been more of a punishment than a treatment. In most cases, heroin addicts that receive any kind of help are rounded up and sent to military detoxification centers where they are thrown into barracks and forced to withdraw from drugs cold turkey with the help of herbal medicines, accupuncture and heavy labor. The addicts then spend three months living in cells, sleeping on mats and eating gruel passed through a hole in their cell door. Sometimes women addicts are accompanied by their children in the cells.
There are 600 compulsory detoxification facilities run by the police plus tougher re-education centers run by the Justice Department for repeat offenders. Both are military-lilke facilities that include manual labor as part of their treatment. In addition to these there are 200 voluntary drug rehab centers.
The main treatment center near Kunming is run by the police and is home to around 2,000 addicts. The program there is regarded as one of the most progressive in China. Addicts go through a three month program in which they spend their days doing calisthenics, marching around the campus, making plastic bags, washing clothes, singing in a chorus, and attending lectures about hygiene and drug laws by white-coated doctors in a room with the slogan “Resolutely Fight the Damage from Drugs” written on the wall. Methadone is provided for a week to 10 days if needed. Addicts have to pay $725 to cover the costs of their stay and make toy dolls puppets dressed in local minority costumes to earn money. They grow tomatoes and raise pigs so they have skills when they get out.

Chinese prison
The treatment centers have spotty records. Studies have show that 85 percent of addicts at the Kunming center go back to heroin, compared to around 75 percent at treatment centers in the United States. Often the people who run the institutions are interested most in making profits off the products the addicts make. Drug users say there are often able to buy drugs from guards
Some villages have formed anti-drug brigades, which use tough love techniques mixed with some sympathy and understanding. Some villages have reported a 40 percent success rate. Their education campaign includes drawing skulls and poppy flowers on school blackboards and playing a boomboxes until crowds shows up and then singing anti-drug songs.
Medications Used to Treat Heroin Addiction
Medicines to help people stop using heroin include buprenorphine and methadone. They work by binding to the same opioid receptors in the brain as heroin, but more weakly, reducing cravings and withdrawal symptoms. Another treatment is naltrexone, which blocks opioid receptors and prevents opioid drugs from having an effect. A NIDA study found that once treatment is initiated, both a buprenorphine/naloxone combination and an extended release naltrexone formulation are similarly effective in addiction. Because full detoxification is necessary for treatment with naloxone, initiating treatment among active users was difficult, but once detoxification was complete, both medications had similar effectiveness. [Source: National Institute on Drug Abuse, National Institutes of Health, U.S. Department of Health and Human Services]
Scientific research has established that pharmacological treatment of opioid use disorder increases retention in treatment programs and decreases drug use, infectious disease transmission, and criminal activity. When people addicted to opioids like heroin first quit, they undergo withdrawal symptoms (pain, diarrhea, nausea, and vomiting), which may be severe. Medications can be helpful in this detoxification stage to ease craving and other physical symptoms that can often prompt a person to relapse. The FDA approved lofexidine, a non-opioid medicine designed to reduce opioid withdrawal symptoms. While not a treatment for addiction itself, detoxification is a useful first step when it is followed by some form of evidence-based treatment.
Medications developed to treat opioid use disorders work through the same opioid receptors as the addictive drug, but are safer and less likely to produce the harmful behaviors that characterize a substance use disorder. Three types of medications include: (1) agonists, which activate opioid receptors; (2) partial agonists, which also activate opioid receptors but produce a smaller response; and (3) antagonists, which block the receptor and interfere with the rewarding effects of opioids. A particular medication is used based on a patient’s specific medical needs and other factors.
Currently, far fewer people receive Medication-assisted treatment (MAT) than could potentially benefit from it. Nearly all U.S. states have higher rates of opioid abuse and dependence than their buprenorphine treatment capacity, and fewer than 1 million of the 2.5 million Americans who abused or were dependent on opioids in 2012 received MAT. Removing barriers to MAT access and utilization is a top priority for the U.S. Department of Health and Human Services and is a key objective of the Secretary’s Opioid Initiative to combat opioid drug-related dependence and overdose.
Methadone
Keth in the 1990s Treatment for heroin addiction usually involves giving addicts a substitute for the opiate drug. Methadone, the most widely used treatment drug for heroin addiction, works in the humans almost the same that opiates do. A reddish liquid used since the mid-1960s to treat heroin addiction, it mitigates the craving for heroin by binding to the brain receptors that usually respond to opiates.
Methadone (Dolophine or Methadose) is a slow-acting opioid agonist. Methadone is taken orally so that it reaches the brain slowly, dampening the "high" that occurs with other routes of administration while preventing withdrawal symptoms. Methadone has been used since the 1960s to treat heroin use disorder and is still an excellent treatment option, particularly for patients who do not respond well to other medications. Methadone is only available through approved outpatient treatment programs, where it is dispensed to patients on a daily basis. [Source: National Institute on Drug Abuse, National Institutes of Health, U.S. Department of Health and Human Services, June 2018]
Methadone is advantageous because it can be taken orally and its effects last so long, up to 24 hours from a single dose. It makes addicts feel a warm glow but not high enough to impair their ability to function fairly normally. It wards off the craving for opiates and mitigates withdrawal. But Methadone is not without its problems. It too is addictive and can be dangerous at high doses. There are hundreds of death from methadone overdoses in the United States every year. In the state of Florida alone, the number of methadone-related deaths rose from 209 in 2000 to 357 in 2001 to 254 in the first six months of 2002. Methadone has become increasingly popular as a street drug. Addicts take when the can’t get other drugs. Doctors sometimes prescribe if for pain relief.

Keith in 2008
Some scientists are opposed to drugs like methadone because using methadone simply replaces one addiction with another. Some addicts continue taking methadone for more than 20 years and regard the drug as medicine for a chronic condition like a blood-pressure-reducing drug. A study by a team led by Prof. David Nutt of Britain’s Bristol University published in the British medical journal Lancet ranked street methadone as the world’s forth most dangerous drug after heroin, cocaine and barbiturates.
New Treatments for Heroin Addiction
Other methadone-like synthetic narcotics used to treat heroin addiction include buprenorphine, Naltrexone and levomethadyl acetate.
The bark of the “Tabernanthe iboga” is a powerful hallucinogenic being investigated a cure for heroin addiction. Found in the rain forests of Gabon and used in initiation rituals of the Bwiti people, it produces a powerful 36-hour trip filled with living dreams and jolting self- realization experiences. Heroin addicts who have tripped on the bark say they had no desire to do heroin after the experience was over. Cocaine addicts have been treated with a drug made from the bark called ibogaine.
“Rapid detox” is a relatively new technique used in the West to treat addicts. Addicts undergoing treatment are given an opiate antagonist to produce acute withdrawal while their extreme discomfort is relieved with a general anesthesia. The procedure is very controversial because it is expensive and risky. Several patients have died. Many doctors feel it is unnecessary and does not address the relapse problem.
Addiction is now widely seen as a disease of the brain in the same way that pneumonia is viewed as a disease of the lungs. It is believed that in the not too distant future, treating addiction will not be any different than treating other chronic, relapsing diseases. Campral is one drug used too fight the long term craving for drugs Rimonabant is a drug that has shown promise treating drug addiction, alcoholism smoking and eating too much. In some places in Canada, addicts are simply given pharmaceutical-grade heroin in an effort to get them to give up crime and prostitution to support their habit.
Buprenorphine

Keith in 2012 Buprenorphine (Subutex) is a partial opioid agonist. Buprenorphine relieves drug cravings without producing the "high" or dangerous side effects of other opioids. Suboxone is a novel formulation of buprenorphine that is taken orally or sublingually and contains naloxone (an opioid antagonist) to prevent attempts to get high by injecting the medication. If a person with a heroin use disorder were to inject Suboxone, the naloxone would induce withdrawal symptoms, which are averted when taken orally as prescribed. [Source: National Institute on Drug Abuse, National Institutes of Health, U.S. Department of Health and Human Services]
Buprenorphine acts an agonist at lower does and antagonist at higher doses. It is similar to methadone with a couple of advantages: it lasts longer, is less intoxicating, is easier withdraw from, and is almost impossible to overdose on. Lasting for about three days per dose, buprenorphine block receptors, not only reducing withdrawal and the craving for heroin and other opiates but also making it difficult t get off on opiates during the three days it is working. In France, buprenorphine has been available for over a decade and is credited with helping many addicts kick and reducing the deaths by heroin and other opiates by 80 percent.
The FDA approved buprenorphine in 2002, making it the first medication eligible to be prescribed by certified physicians through the Drug Addiction Treatment Act. This approval eliminates the need to visit specialized treatment clinics, thereby expanding access to treatment for many who need it. Additionally, the Comprehensive Addiction and Recovery Act (CARA), which was signed into law in July 2016, temporarily expands prescribing eligibility to prescribe buprenorphine-based drugs for medication-assisted treatment to qualifying nurse practitioners and physician assistant. In February 2013, FDA approved two generic forms of Suboxone, making this treatment option more affordable. The FDA approved a 6-month subdermal buprenorphine implant in May 2016 and a once-monthly buprenorphine injection in November 2017, which eliminates the treatment barrier of daily dosing.
Naltrexone and Vivitrol
Naltrexone is an antagonist that blocks the effect of heroin and opiods on the brain's receptors. It is not addictive or sedating, and does not result in physical dependence; however, patients often have trouble complying with the treatment, and this has limited its effectiveness. In 2010, the injectable long-acting formulation of naltrexone (Vivitrol) received FDA approval for a new indication for the prevention of relapse to opioid dependence following opioid detoxification. Administered once a month, Vivitro may improve compliance by eliminating the need for daily dosing. [Source: National Institute on Drug Abuse, National Institutes of Health, U.S. Department of Health and Human Services]
Naltrexone is a strong drug that sends an untreated addict immediately into withdrawal and is used mainly to prevent former addicts from relapsing. Users don't like it because a dose last a day and make them feel anxious and unhappy. Because of this many quit. Vivitrol came on the market in 2006. It blocks the effects of a drug but doesn’t stop the withdrawal symptoms. The legs of patients who take it often swell up to twice their size after the drug is taken. During the weeks that follow they endure nasty withdrawal symptoms but are unable to get any relief from the abused drug or alcohol. After withdrawal is completed patients keep taking Vivitrol. Relapse is unlikely to happen as patient will not get high when they take the drug.
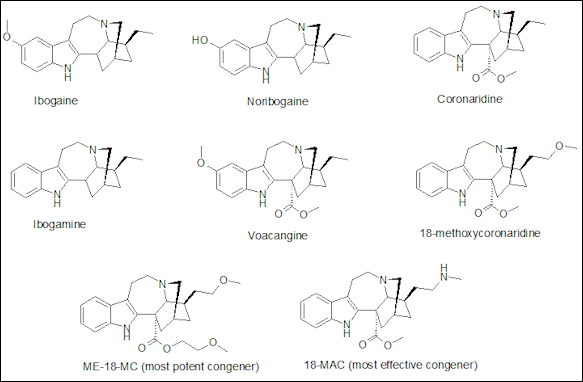
Iboga alkaloids
Image Source: Wikimedia Commons; DEA (Drug Enforcement Administration)
Text Sources: 1) “Buzzed, the Straight Facts About the Most Used and Abused Drugs from Alcohol to Ecstasy” by Cynthia Kuhn, Ph.D., Scott Swartzwelder Ph.D., Wilkie Wilson Ph.D., Duke University Medical Center (W.W. Norton, New York, 2003); 2) National Institute on Drug Abuse, National Institutes of Health, U.S. Department of Health and Human Services; 3) United Nations Office on Drugs and Crime (UNODC) and 4) National Geographic, New York Times, Washington Post, Los Angeles Times, Wikipedia, The Independent, Times of London, The New Yorker, Time, Newsweek, Reuters, Associated Press, AFP, , Lonely Planet Guides, and various books and other publications.
Last updated April 2022
