CHOLERA
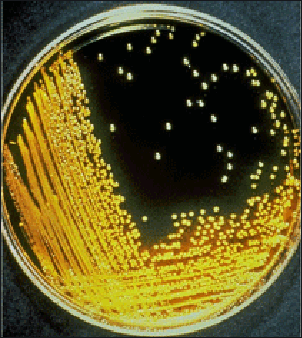
cholera bacteria
in a petri dish Cholera is an acute intestinal infection caused by a comma-shaped bacterium called “Vibrio cholerae” O-group 1. It is highly contagious and causes a copius, painless, watery diarrhea that can quickly lead to severe dehydration and death if not treated promptly. The bacterium is excreted through the feces. One of the most common ways to get it is to drink water contaminated by the feces of victims of the disease. [Source: Steven Shapin, The New Yorker , November 6, 2006]
The “vibrio cholerae “O-group 1 bacterium lives in close association with zooplankton, particularly minute crustaceans known as copepods. It is not unusual for a single copepod to provide a home for 10,000 “vibrio cholerae” , enough bacteria to cause the disease. The bacterium produces a toxin that causes diarrhea and severe fluid loss.
Cholera now kills about 5,000 people a year. In the Middle Ages it killed maybe million people a year and continued being a major killer in Europe until the 19th century when its connection with contaminated water was discovered and incidence of the disease was greatly reduced with improved sanitation. In 1991 cholera came to Latin America for the first time since 1895. New strains have appeared in India, Bangladesh and other parts of Asia.
Cholera is now largely regarded as a developing world disease, often occurring in the wake of natural disasters and civil wars. In 2004, the Center for Disease Control reported only five cases in the United States, four of which were acquired abroad. In the past few years outbreaks have occurred in Angola, Sudan, the Democratic Republic of Congo, Senegal and Niger. In the early 1990s there were large outbreaks after floods in Bangladesh and India and after the genocide in Rwanda and more than a million cases in Latin America. [Source: Steven Shapin, The New Yorker , November 6, 2006]
Websites and Resources Centers for Disease Control and Prevention (CDC) cdc.gov/DiseasesConditions ; World Health Organization (WHO) fact sheets who.int/news-room/fact-sheets ; National Institute of Health (NIH) Library Medline Plus medlineplus/healthtopics ; Merck Manuals (detailed info many diseases) merckmanuals.com/professional/index
Cholera Causes
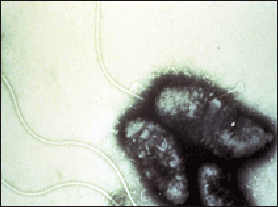
cholerae bacteria
Cholera is usually caused by contaminated water or seafood. Sometimes it results from the use of human excrement for fertilizer or the flooding of lakes in which raw sewage has flowed into. Cholera outbreaks sometimes occur after unusually warm ocean waters and coastal algae blooms.
Cholera often occurs after a massive flood when decomposed bodies and large amounts of sewage enter the water. But there are also plenty of examples of bodies decomposing in the water and more sewage than usual in which no cholera occurs.
Once it has taken hold cholera can spread with terrifying and thorough quickness, often infecting all the houses in a neighborhood as it advances. Nineteenth century outbreaks in Europe were described like approaching storms with weather-report-like reports. During a 1831-32 epidemic that struck Paris the poet Heinrich Heine wrote that it “was like the end of the world had come.” The people fell on the victims “like a beast, like maniacs.”
Cholera Symptoms
The cholera infection produces "rice-water" diarrhea, and sometimes causes a fever and headache. It is often mild and does not require hospitalization but at the same it can be very serious. The diarrhea can cause victims to lose as much as eight liters of body fluids a day and kill quickly by causing severe dehydration. What is also worrisome about the disease is that it is highly infectious.
Cholera comes on quickly and accelerates through it symptoms equally fast. The first signs is explosive “rice water” diarrhea that sometimes has a fishy smell. The bits of white in stool is the linings of the small intestine. The diarrhea is often accompanied by frequent vomiting. Both can dehydrate a victim quickly with the dehydration often causing sunken eyes, painful cramps, leathery skin, low blood pressure, and an irregular heartbeat. [Source: Steven Shapin, The New Yorker , November 6, 2006]
A mid-19th century report of cholera described victims who were “one minute warm, palpitating human organism — the next a sort of galvanized corpse, with icy breath, stopped pulse, and blood congealed — blue, shriveled up, convulsed.” What is particularly nasty is that the mind remains alert through it all. The “mind within remains untouched and clear, shining strangely through the glazed eyes...a spirit, looking out in terror inside from a corpse.”
Cholera Prevention and Treatment

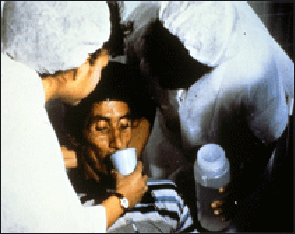
treating cholera
patients in Peru The best way to avoid cholera is wash with soap and be careful about what you eat and drink (See Food and Water Precautions Above). After a natural disaster such as flood when cholera is a concern and clean water is in short supply local water supplies are cleaned through “flocculation,” a process that involves adding a solution to congeal dirt particles so they can be filtered out, and adding chlorine to kill the germs.
The cholera vaccine is only 50 percent effect and is not recommended by doctors. Most countries that once required a cholera vaccine no longer do. Improved oral vaccination may be available soon.
Cholera can be easily be treated immediately with solution of oral dehydration salts or lots of fluids and electrolytes. Those that are severely dehydrated need intravenous fluids and antibiotics. Treated patients have a survival rate of 99 percent.
If you think you may have cholera seek medical attention immediately. As symptoms appear take steps to prevent dehydration. Person with severe cases usually respond dramatically to simple fluid- and electrolyte-replacement therapy (drinking lots of fluids and take replacement salts). In the hospital the treatment consist mainly of intravenous therapy. Cholera is resistant to all antibiotics.
The genome of the bacteria that causes cholera has been figured out. This discovery may help produce a better vaccine and/or better treatment.
History of Cholera
The word “cholera” is derived from “choler”, the Greek word for yellow bile. Hippocrates described cholera as a post-childhood disease that could be treated by eating goat meat (most likely he was talking about a milder form of diarrhea). The potent life-threatening disease that we know emerged from India in 1817. A pandemic in the early 1820s reached Southeast Asia, east Africa, the Middle East and the Caucasus before dying out in 1823. A second powerful, widespread and devastating pandemic occurred between 1826 and 1837 again began in India and spread to Europe and America, killing hundred of thousands before it ran its course. [Source: Steven Shapin, The New Yorker , November 6, 2006]
Cholera became a serious problem when the world became more urbanized and industrialized in the 19the century. Before that epidemic tended to occur in localized areas and not travel very far. A cholera epidemic in London in 1848 killed 14,600 people.
The cholera bacterium “Vibrio cholerae” was discovered by German physician Robert Koch in 1883. In the first part of the 19th century it was widely believed that the disease was caused by noxious effluvia — bad air possibly from the — the bowels of the earth. It was not thought of as contagious, rather it struck certain areas because al the people breathed in the same bad air. The poor were victimized more because of their filthy, immoral way of life and perhaps because the noxious airs emerged from the earth in their neighborhoods, as the horrible smells there testified. Remedies included wearing flannel, dousing oneself and masking the smell with camphor vapors and smothering one’s food with garlic along with praying and fasting. Neighborhood-wide strategies included burning tar, sugar and vinegar and dousing the streets with lime or chlorine.
Family Lost to Cholera in Manchester 1832

notice at Haiti outbreak Describing cholera in Manchester in 1832, Sir James Kay-Shuttleworth wrote: "On my arrival in a two-roomed house, I found an Irishman lying on a bed close to the window. The temperature of the skin was somewhat lower than usual, the pulse was weak and quick. He complained of no pain. The face was rather pale, and the man much dejected. None of the characteristic symptoms of cholera occurred, but his attendant told me that his strength had gradually declined during the day, and that, seeing no cause for it, he had formed a suspicion of contagen.”
"I sat by the man's bed for an hour, during which the pulse became gradually weaker. In the second hour it was almost extinct, and it became apparent that the patient would die ...As twilight came on the sufferer expired without cramps or any other characteristic symptom...The wife had been soothed and she readily consented to be removed with her children to the hospital...None of them showed any sign of the disease, and I left to the ward to take some refreshment. On my return, or at a later visit before midnight, the infant had been sick in the mother's arms, had made a faint cry and died...While I was there the children did not wake...and at length I thought I might myself seek some repose."
"When I returned about six o'clock in the morning, another child had severe cramps with some sickness, and while I stood at the bedside, it died. Then, later, the third and eldest child had all the characteristic symptoms of cholera and perished in one or two hours. In the course of the day the mother likewise suffered from a severe and rapid succession of the characteristic symptoms and died, so that within twenty-four hours the whole family was extinct."
Finding the Source of Cholera
In the late 1840s and early 1850s, an English physician named John Snow traced the course of a cholera outbreak in London and helped bring the outbreak to an end. London at time was a very dirty and unsanitary place. "We live in muck and filth. We ain't got no privies, no dust bins, no drains, no water supplies in the whole place...We all suffer, and numbers are ill, and if the Cholera comes Lord help us," a group of poor wrote to the London Times at the time. [Source: Steven Shapin, The New Yorker , November 6, 2006]
cholera treatment Snow was an anesthetist and founding member of the London Epidemiological Society. He administered the gas to Queen Victoria in the first chloroform-assisted royal birth. His quest to understand cholera began during a serious cholera epidemic in 1848 when he began studying where outbreaks of the disease occurred and where people got their water.
In 1854 another major cholera epidemic broke out. In a move that would change the nature of science, Snow plotted the cholera deaths on a map and figured out the source of the disease was water from a particular well. How was the epidemic stopped? The handle on the well was removed. Some credit Snow with being the world’s first epidemiologist. Although the magnitude and breadth of his discovery took some years to be accepted and appreciated it lead to changes in the ways diseases were tackleed and prevented and saved hundreds of thousands of lives.
Book: “The Ghost Map: the Story of London’s Most Terrifying Epidemic-and How It Changed Science, Cities and the Modern World” by Steven Johnson (Riverhead Books, 2006).
Image Source: Centers for Disease Control and Prevention cdc.gov/DiseasesConditions
Text Sources: Centers for Disease Control and Prevention (CDC), U.S. Department of Health and Human Services; World Health Organization (WHO) fact sheets; National Geographic, New York Times, Washington Post, Los Angeles Times, The New Yorker, Time, Reuters, Associated Press, AFP, Lonely Planet Guides and various websites books and other publications.
Last updated May 2022
